 Sphincter of Oddi dysfunction (SOD) is a functional gastrointestinal abnormality which commonly causes acute pancreatitis. Even without the unfortunate occurrence of acute pancreatitis Sphincter of Oddi dysfunction is characterized by pancreatobiliary pain that can be debilitating and impair the patients quality of life.
Sphincter of Oddi dysfunction (SOD) is a functional gastrointestinal abnormality which commonly causes acute pancreatitis. Even without the unfortunate occurrence of acute pancreatitis Sphincter of Oddi dysfunction is characterized by pancreatobiliary pain that can be debilitating and impair the patients quality of life.
As far as I can tell from reading dozens of articles nobody knows for sure what causes this functional abnormality.
Sphincter of Oddi dysfunction is associated with gallbladder disease, gallstones and ironically those who have the gallbladder removed seem to be more prone to Sphincter of Oddi dysfunction.
The majority of SOD patients are female, 30 – 50 years of age; however, that certainly doesn’t mean that males are immune to this condition. Close to 20% of the lucky folks with Sphincter of Oddi dysfunction are male.
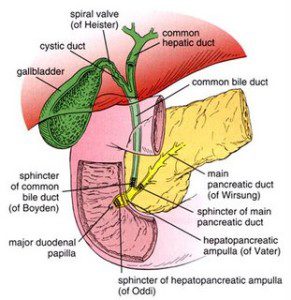
What Is The Sphincter of Oddi?

Sphincter of Oddi
Imagine a strong doughnut, a muscular valve that surrounds the exit of the bile and pancreatic ducts, into the duodenum, right at the papilla of Vater [1,2]. That muscular valve is called the Sphincter of Oddi.
The SO is normally closed for business. It opens only in response to the flow of digestive juices after a meal so that those digestive juices can enter the duodenum and help digest the foods eaten for intestinal absorption to occur.
The mechanism of Sphincter of Oddi dysfunction, why it occurs, is not well-known. The theory is that the sphincter goes into a spasm causing a temporary back-up of biliary and pancreatic juices. This “back-up” is not a good thing.
Sphincter of Oddi Dysfunction Symptoms
The back-up of digestive juices we were talking about previously, results in abdominal pain. The pain can be mild, moderate or severe, even debilitating. Unfortunately this back-up of digestive juices can and commonly does cause acute pancreatitis.
Symptoms of SOD include:
- abdominal pain
- located in mid- or right-upper abdomen
- might also be felt in the back and shoulders
- can last anywhere from several minutes to several hours
- can be a mild, dull throbbing pain, or …
- can be so severe that the individual is incapacitated
- Nausea with or without vomiting
- Fever
- Chills
- Diarrhea
- jaundice
- prolonged obstruction may result in bile leaking back into the blood stream
- results in abnormalities of the liver function tests
- can result in a yellowish discoloration of the eyes and skin
The above symptoms can come and go. They can be mild one time and severe the next.
https://www.youtube.com/watch?v=KBJkzciCOgo
Diagnosing Sphincter of Oddi Dysfunction
 Chances are that unless you have a really sharp doctor you’ll suffer for months, even years, playing let’s find the clue, especially if you are male, have NOT had any sign of gallbladder disease or had gallbladder disease and underwent cholescystectomy (gallbladder surgery). If on the other hand if you are female, between 30 and 50 and have had your gallbladder removed your chances of having your doctor’s light bulb flash on Sphincter of Oddi dysfunction is much higher.
Chances are that unless you have a really sharp doctor you’ll suffer for months, even years, playing let’s find the clue, especially if you are male, have NOT had any sign of gallbladder disease or had gallbladder disease and underwent cholescystectomy (gallbladder surgery). If on the other hand if you are female, between 30 and 50 and have had your gallbladder removed your chances of having your doctor’s light bulb flash on Sphincter of Oddi dysfunction is much higher.
When Sphincter of Oddi dysfunction is suspected by your doctor, he or she will most likely run tests to check for other conditions that might be causing your abdominal pain. It is important to rule out biliary cancer, cancer of the pancreas, liver, peptic ulcer or stones in the ducts that carry bile from the liver. In some cases even heart conditions can cause pain that seems to be originating from the abdomen.
Initial investigations:
- Blood is drawn to check on liver and pancreas tests (particularly alkaline phosphatase, transaminases and amylase/lipase).
- Standard ultrasound and CT scans are used to look for structural causes, but are not completely accurate.
- When these are unrevealing, most experts recommend other imaging procedures, such as Magnetic Resonance Cholangiopancreatography (MRCP) and Endoscopic Ultrasound (EUS). One of these should be used before considering more invasive, risky procedures like ERCP with Sphincter of Oddi manometry to check sphincter pressure.
- Another test (HIDA scanning) is sometimes used to detect poor emptying of the bile duct due to sphincter activity, and BOTOX injection into the sphincter has been explored as a test for over-activity.
- Sphincter of Oddi manometry is done by placing a small tube into your pancreatic duct or common bile duct near the SO to measure how well it is contracting and expanding. There is a risk of acute pancreatitis with this test [3].
 What are the criteria your doctor may be looking for via tests and patient history in order to correctly diagnose Spincter of Oddi Dysfunction? Let us take a peek …
What are the criteria your doctor may be looking for via tests and patient history in order to correctly diagnose Spincter of Oddi Dysfunction? Let us take a peek …
Type I: All of the following:
- Recurrent biliary pain
- Liver test elevations (AST or ALT) on two separate occasions (2x upper limit of normal) with resolution inbetween
- Dilated common bile duct (11 mm)
Type II:
- Recurrent biliary pain plus 1 of the above criteria
Type III
- Biliary type pain only
Type III is the probably most difficult to diagnose because there are no physical signs that show on tests. So they have to listen closely to the patient and many of us know how difficult that is for doctors 🙂
Sphincter of Oddi Dysfunction Treatment
 Sphincter of Oddi dysfunction treatment can be a crap shoot. In those people who do not have severe symptoms sphincter of oddi dysfunction treatment may be drugs that reduce pain and help prevent sphincter of oddi spasms. In others with severe symptoms the doctor may refer them to a surgeon for a procedure called a sphincterotomy.
Sphincter of Oddi dysfunction treatment can be a crap shoot. In those people who do not have severe symptoms sphincter of oddi dysfunction treatment may be drugs that reduce pain and help prevent sphincter of oddi spasms. In others with severe symptoms the doctor may refer them to a surgeon for a procedure called a sphincterotomy.
There are 3 categories of Sphincter of Oddi dysfunction, (1, 11, 111). Each category of Sphincter of Oddi dysfunction suggests certain forms of Sphincter of Oddi dysfunction treatment. I will give my unprofessional Sphincter of Oddi dysfunction treatment ideas (what I would do if I had SOD) that should probably never be used, especially without your doctors approval because let’s face it – I am not a doctor, not an expert, not even a highly educated quack!
What Is Sphincterotomy?
Sphincterotomy is a difficult, delicate procedure. To make a long story short they put you to sleep, run a tube (with a blade) down your throat, into your common bile duct, down past your pancreatic duct to the sphincter found at the enterance to your duodenum. Then the surgeon cuts your sphincter. The video will show you what happens. Now this is a DUAL sphinchterotomy which includes doing the pancreatic duct as well which in my opinion (which isn’t and educated opinion) would almost guarantee or at least increase the probability, substanially, that the woman will later experience acute pancreatitis.
 Sphincterotomy carries a fairly high risk of complications. 5% – 15% of patients experience complication [4,5]. Acute pancreatitis (mild, moderate or severe) is one of the possible and most common complications. Other complications include hemorrhage, perforation, cholangitis, cholecystitis, death and various other issues. In one study of 2347 patients, 229 (9.8 percent) had a complication, including pancreatitis in 127 (5.4 percent) and hemorrhage in 48 (2.0 percent). There were 55 deaths from all causes within 30 days; death was directly or indirectly related to the procedure in 10 cases [4]. The sad part is that sphincterotomy only works on about 50% of those who have it done. In my opinion it is a dangerous crap shoot.
Sphincterotomy carries a fairly high risk of complications. 5% – 15% of patients experience complication [4,5]. Acute pancreatitis (mild, moderate or severe) is one of the possible and most common complications. Other complications include hemorrhage, perforation, cholangitis, cholecystitis, death and various other issues. In one study of 2347 patients, 229 (9.8 percent) had a complication, including pancreatitis in 127 (5.4 percent) and hemorrhage in 48 (2.0 percent). There were 55 deaths from all causes within 30 days; death was directly or indirectly related to the procedure in 10 cases [4]. The sad part is that sphincterotomy only works on about 50% of those who have it done. In my opinion it is a dangerous crap shoot.
Of course, as always, if you have been diagnosed with Sphincter of Oddi dysfunction you need to determine what treatment is right for you. I need you to complete understand that I am NOT giving you advise. I’m giving you information along with my uneducated opinions. You need to do your own research and ask your doctor a lot of direct, pertinent questions. However …
If it were me I think I’d choose a safer route first, especially since SOD has been found to respond to a low fat diet just as do pancreatitis and gallbladder disease. I’d probably also use grape seed extract and grape fruit seed extract (or juice) not only to help relieve symptoms by decreasing any inflammation but to also help protect the pancreas from acute pancreatitis.
Sphincter of Oddi Diet – I Have SOD What Can I Eat Safely?
 I imagine many people who suffer from sphincter of Oddi Dysfunction often wonder “I have SOD what can I Eat Safely?”
I imagine many people who suffer from sphincter of Oddi Dysfunction often wonder “I have SOD what can I Eat Safely?”
If you read what others write about a diet for sphincter of oddi dysfunction you’ll read “No” because all people are different. That there is no perfect SOD diet because people are all different and …
This is true to the extent that there are 3 types or classifications (1,11,111) of sphincter of oddi dysfunction which probably (I’n guessing here) determine what foods are or are not acceptable. There really isn’t any concrete, irrefutable knowledge when it comes to a perfect SOD diet. Yet …
I believe, in tackling SOD as I have pancreatitis via diet and supplements, there are certain points one can take as irrefutable when looking to perfect a sphincter of oddi dysfunction diet. Points that will help the largest number of people realize relief, even a “remission” of symptoms for a period of time.
One irrefutable point is that ALL biliary disease responds to a low fat diet. According to the Yale School of Medicine and John Hopkins SOD responds to a low fat diet.[6,7] When one reads that infamous schools of medicine actually say something, thought of as non-medical, such as diet, actually helps a condition improve the reader should most likely listen. Yet …
High Fat foods may NOT be the only food type that creates symptoms.
The reason foods may create symptoms is because of increased bile flow. Increased bile flow from the liver to the gallbladder may cause the gallbladder to release more bile and/or any stones and sludge that may also be harbored within the gallbladder itself.
If there are stones or sludge within the gallbladder increased bile flow could spark gallbladder inflammation, cause the stones and sludge to pass which could also cause gallstone pancreatitis (not good) and/or cause the sphincter of oddi to “spasm” and in trun cause more pain, symptoms or acute pancreatitis. None of the above is good. Yet …
Stagnant bile can also cause problems such as gallstone formation, even inflammation and infection so it’s a “catch 22” isn’t it? So seriously …
What Foods Should Be Avoided When You Have SOD?
 1) Any foods high in fat. The list is long but here is a partial list: Beef, pork, lamb, duck, goose,processed meats egg yolk, butter, mayo, margarine, cooking oil, olive oil, oil. Also …
1) Any foods high in fat. The list is long but here is a partial list: Beef, pork, lamb, duck, goose,processed meats egg yolk, butter, mayo, margarine, cooking oil, olive oil, oil. Also …
Nuts (all kinds), avocado, coconut, peanut butter, pastries (doughnuts, cake, cookies, pie, etc). Processed foods (soups, drinks, fast foods) are another source of hidden, high fat. High fat foods, whether those fats are “good fats” or “bad
fats” irritate components of the digestive system (liver, gallbladder, pancreas, and the sphincters).
High fat foods cause increased amounts of bile to flow. Yet …
Any foods are going to cause bile to flow because bile, along with pancreatic juice, help digest foods we eat. So, as with pancreatitis, patients with SOD should learn to eat to live versus living to eat. Food is NOT your friend.
I should point out at this juncture that doing a food diary is essential to determine exactly what foods you tolerate and those you do not tolerate well. And you should avoid all foods that you do not tolerate. There is only ONE way that I know of for sure to find out which foods other than those already listed that you do or don’t tolerate and that is by doing a food diary with the initial prep.
Without the prep you may as well not even do a diary. Cleansing your digestive tract of ALL food, whether offensive or not (which at this point you don’t know for sure), is imperative to success.
 The East Indian spice Turmeric increases bile flow. It increases it enough that SOD patients should probably avoid it along with curcumin which is concentrated curcuminoids and is made from the turmeric root. Avoid foods made with turmeric (curries, sauces, mustard).
The East Indian spice Turmeric increases bile flow. It increases it enough that SOD patients should probably avoid it along with curcumin which is concentrated curcuminoids and is made from the turmeric root. Avoid foods made with turmeric (curries, sauces, mustard).
Other foods implicated for an increased release of bile include:
- Honey
- Radish
- Celery
- Carrot
I find it hard to believe that honey, radish, celery and carrot can be offensive but who knows? How correct the implications are I have no clue because I have searched and searched for information (concrete scholar type) and have found very little. So, I am going to say this again …
If you have been diagnosed with sphincter of oddi dysfunction food is not your friend and you need to do a food diary, including the proper prep before starting!
What Else Should I Avoid If I Have Sphincter of Oddi Dysfunction?
 Before there was ERCP with manometry physicians used to use what was called the Nardi Test. It was simply a test that involved two drugs. Morphine and prostigmine. This helped them diagnose SOD in the earlier days. The test has now been discontinued. But …
Before there was ERCP with manometry physicians used to use what was called the Nardi Test. It was simply a test that involved two drugs. Morphine and prostigmine. This helped them diagnose SOD in the earlier days. The test has now been discontinued. But …
The fact that morphine makes the Sphincter of Oddi spasm and provocates it, even causing acute pancreatitis in many cases, should give one pause. Abstaining from narcotics especially those derived from morphine would likely be a very good idea. Instead of narcotics I would suggest large doses of grape seed extract, 800 – 1200 mgs of Ibuprofen and a really good nausea medication.
I can speak from experience how NOT fun the Nardi Test is simply because that is how Doctor Langdon diagnosed me with acute pancreatitis. The interesting thing is he never mention sphincter of Oddi Dysfunction but I have often wondered whether or not that was part of my problem. As IF I don’t have enough to contend with lol. That may be the reason narcotics did NOTHING for me and why Ibuprofen works so well in comparison. Even though he didn’t mention it (or if he did I missed it!) yet he prescribe a synthetic anticholinergic agent (Robinul). Who knows? I don’t, not for sure. Yet, if you have been diagnosed with SOD it may be wise to avoid narcotics that seem to aggravate SOD, sphincter of oddi dysfucntion.
References:
1) Papilla of Vater: structure and function – Read here
2) Sphincter of Oddi dysfunction – Read here
3) Complications of sphincter of Oddi manometry: biliary-like pain versus acute pancreatitis – Read here
4) Complications of Endoscopic Biliary Sphincterotomy – Read Here
5) Complications of endoscopic biliary sphincterotomy – Read here
6) Sphincter of Oddi dysfunction: SOD after EPISOD, Now what do we do ? Read here
Priya A. Jamidar, M.D., FASGE
Professor of Medicine,
Director of Endoscopy
Yale School of Medicine
7) Gastroenterology and Hepatology – FAQs about Sphincter of Oddi Dysfunction – Read Here
John Hopkins Medicine
After almost 4 years of severe pain and 11 trips to the ER, many CT scans, MRCP’s, 5 ERCP’s, upper GI’s, stents, stone removal (gallbladder removed 6 years ago), enlarged ducts, sludge, 4 hospital stays following ERCP and doctors just shrugging and saying they have no answers…I am encouraged by this information. I have been in pain almost all of July, latest MRCP shows no stones this time, and I am at the end of my rope…I am 69 and can’t imagine having this pain for the rest of my life. I am not sure what to do next but hope your information will help me in trying to find answers and solutions and what I can do to improve my quality of life…this pain is non stop.
Hi Linda – I am sorry you are ill and in pain. I have been there. It sucks. Did you have gallstones? Is that why they took out your GB or do you have pancreas calcification? I’m asking what kind of stones.
You know, I do not have a lot of clarity about my condition. I had all sorts of gallbladder tests at the University of CA Davis in 2002-2004 and all tests for gallbladder were negative. So in 2009 when they removed it, I was surprised. I didn’t present with typical gallbladder symptoms.The surgeon believed a 2003 ERCP left my bile duct with an opening that got infected so after the Gall bladder surgery they kept me for 4 days to clear up the infection. I never remembered a comment about stones back then. I was going over my ER reports last night and they all just say that I came in with severe pain, they did blood work, CT scan, and eventually gave me enough medication to stop the pain and sent me home. Out of the last 4 ERCP’s, I was hospitalized with severe pain 3 times, kept a few days and sent home but no one ever gave me a diagnosis or mentioned pancreatitis. I have 15 bottles of various strengths of codeine and only 1 doctor mentioned SOD as a possibility. I generally have a few days of constant pain and a few days of relief…but I think the doctors just think I am an old complaining woman who wants attention.
Linda, all I can say is I hope you don’t have SOD. You definitely could (symptoms etc) and I find it really interesting that one of your doctors had that thought. He/she must be on the ball. Anyway if you do have it there are 3 classifications (1,11,111). Class 1 and 11 are supposedly the more severe forms BUT like the pancreas and gallbladder the SO also responds to a low fat diet and elimination of “trigger” foods. Unfortunately SOD has more “trigger” foods than pancreatitis. Curcumin (from the East Indian Turmeric root), for example, which a is great natural remedy for pancreatic pain and symptoms causes bile to flow more substantially and more bile flow seems to cause the SO to spasm in many people, which in turn causes symptoms and even acute pancreatitis. So doing your own food diary, including the initial preparation, may be more important than ever so that you are able to determine all trigger foods with certainty in case you really do have SOD. From what I understand any food could be a possible trigger food in SOD patients but those with high fat and those that cause an increase in bile flow (quite a number of foods) are definitely suspect.
Thanks so much for responding. Reading about the 3 types of SOD I fit type 2: On-going severe pain and I have or have had dilated bile ducts. The ER doc who initially suggested SOD said they clipped the SO muscle and he doesn’t know why doctors do that because of the problems it causes. My pain is so random. Yesterday I happened to not have breakfast or lunch due to being super busy and when I laid down for a nap around 1 I could feel a spasm wanting to start and yep…got 2. These remind me of leg cramps…to make it stop I sort of bear down, and push my belly out as hard as I can and then I take a nitro! (One of my helpers) When I finally did eat dinner, as usual, half way through I started to hurt which happens almost every dinner. 90% of my 10 ER visits have been after 10pm and the ER is behind our house but within 15 minutes of the initial pain, I am nearly screaming in pain by the time I get to the ER. I hate taking Codeine but when it gets that bad it is all I can do to avoid another 6 hour ER stint! I live in Roswell, NM and we are lucky to have one gastro doc and no one who knows much of anything about my condition. They all just tell me I am one of the unlucky ones who got this problem after ERCP…some days I just feel like taking all of my meds which is a scary thought to have. Due to finances I have to use up the groceries I have then do a cleanse and then start the food diary. Meanwhile I am avoiding fats and oils and making sure I am being cautious with the foods I am using up. You have been so helpful. Glad you clarified about Curcumin as I was about to order it.
Linda – You are welcome but I’m concerned. You said “some days I just feel like taking all of my meds which is a scary thought to have.” THAT is NOT the solution. I have been where you are. Daily pain, nausea, then horrible pain. 3 years of total nightmare. I’ve had almost 62 years of on and off crap. So trust me when I say I know what it’s like. Since I am a Jesus follower and child of the most high God the Bible tells me …
“So we are always confident, knowing that while we are at home in the body we are absent from the Lord. For we walk by faith, not by sight. We are confident, yes, well pleased rather to be absent from the body and to be present with the Lord.” 2 Corinthians 5:6-8 New King James Version (NKJV) Yet I KNOW there is a reason I am still here and even though it may sound like a good idea at times it isn’t because the Lord determines when our time and presence is no longer needed here on earth. If you have those feelings (suicide) get in contact with someone who is trained to help. Tell your doctor, your Pastor, someone. Heck, call me. My number is on this site. BUT do NOT end your life because it isn’t the right solution. IF you don’t have a relationship with Almighty God you may want to give Him a shout. He is my rock. And when I need comfort He answers. And one other thing …
I know you said the Codeine helps but narcotics often cause the SO to spasm in those who suffer with SOD. What I’m saying is the Codeine may actually be causing a “vicious circle.” When you have bad pain try Ibuprofen just to see if it helps (800 – 1000 mgs). Try smaller doses (200 – 400 mgs) for mild pain. Ibuprofen is not safe (no drug is safe) but it doesn’t cause the SO to spasm. Grape seed extract may also be beneficial. It is non-toxic so you can take a lot and not die.
Linda if you can control your pain and other symptoms, even become pain free more days than not with diet, supplements (daily) and Ibuprofen when necessary your outlook will change and life will again become enjoyable. If I can help holler. 🙂
Thank you, it is encouraging to actually get a reply from someone on the web! I promise I will keep fighting the good fight. I have read about opioid’s backfiring so I am just trying to meditate and watch what I am eating, having water as my beverage of choice and I do have an Rx for Ibuprofen so I will try that. John Hopkins web sight had a LOT of good information on SOD and while going there, (to their facility) is out of the question…I am not sure I would go along with any type of surgery because the idea of them going in for a procedure and coming out in the kind of pain I have had with just an ERCP scares me too much. I am just hoping for an improvement. Thanks again.
You’re welcome Linda 🙂
If you don’t mind me.asking do you have fibromyalgia
Thank you for writing about this.
I had a ruptured appendix at age 15, an ERCP which almost killed me (because of resulting acute pancreatitis), had my gall bladder removed, then pancreatitis 2 more times, and now SOD. Spasms were triggered after taking post-op opiates.
I switched to a whole foods/plant based, dairy-free (I’m allergic to milk), low fat diet two months ago. So far, so good. Time will tell.
Hi HartOfBeck – You are welcome. It sounds like you have had some rough road to negotiate. I’m glad to hear that a change in diet has helped.
Hello,I had a bout of pancreatitis in 2013 ,I was sent home on clear liquid diet on Friday. Had ultrasound on Monday where a stone was stuck in bile duct.Was called back to be admitted to hospital that night,hidascan on Tuesday morning showed no sign of stone so it was said to have passed or dissolved and I was taken straight to OR and gallbladder removed .Since that time I am now in the midst of my 5th bout of what I believe to be Sod and nearing pancreatitis.I am at my wits end as I’ve had all the test at each flare up with no answers as to what is happening to me .I made it 13 months and even was on low carb diet losing weight doing well until a week ago and that dull ache began and ha now progressed to the point I cannot eat because the pain is unbearable.The only thing I did differently was add pyncogenol to my supplement regimen.Is it possible it could have caused increased bile production hence the flare up.I am so grateful I found your sight as the ibuprofen has spared me several trips to er and doctors who don’t seem to be able to help me
Hi Becky I am sorry to hear you are ill. You said “The only thing I did differently was add pyncogenol to my supplement regimen.” True pycnogenol is maritime pine bark extract – is that what you are using? IF so I doubt it would do anything but help because it is very similar to grape seed extract in that it is full of OPC’s which are highly anti-inflammatory. YEARS ago I used to use an incredibly awesome formula that contained pine bark extract, grape seed extract and curcumin in one capsule. It was killer but the company went out of business. Anyway … Anything is possible but I can’t see it doing anything but helping SOD symptoms but one who doesn’t have SOD (me) can never know for sure. I definitely think you should consider fasting to give things (the inflammation if it is there or the sphincter to quit its spasm) to resolve. I definitely wouldn’t use curcumin – just grape seed extract and vit c with ibuprofen while in pain and fast (no food, just water to stay hydrated) and see what happens. There are 3 classes or categories of SOD class 1 and 2 have a commonality and that is a dilated CBD (common bile duct) on CT/EUS/MRI. Class 3 is much harder to diagnose because nothing shows from what I understand and testing the sphincter via ERCP can cause acute pancreatitis. And in any event doctors love to do ERCP in all 3 cases so they can have that sphincter spasm as proof and cause their patient pain, sometimes incredible pain for days/weeks. IF you do have SOD narcotics will cause the sphincter to spasm often causing acute pancreatitis. I hope you do NOT have SOD because it is a bugger to treat. Doctors have no clue how to treat it without endangering the patient. It supposedly responds to a low fat diet but ANY food will cause bile to flow which could irritate the sphincter enough to cause a spasm and the resulting illness, even AP. I know some ladies who have it and suffer with it and not much seems to really help BUT I also don’t believe they follow a strict low fat diet and take the supplements. And it mat be because they tried and it just didn’t help. I don’t know. Again I don’t have it so I can’t say this or that actually helps. 🙁
I am 63 year old female. Had my lap chole over 20 years ago. Unfortunately I had to have an ERCP with sphincterotomy 2 years after gallbladder removed due to stones in common bile duct. I have had right upper quadrant pain off and on ever since. I have had many CT scans and labs. The CT’s usually showed common bile duct dilatation. On my most recent CT it showed mild pancreatic duct dilatation. This freaked me out (I’m a nurse). I went to gastro and had EGD with ultrasound. Showed stones in duct. Had 2nd ERCP (no sphincterotomy). Following day had tremendous abdominal pain, fever, vomiting, elevated liver enzymes (amylase/lipase not elevated). I was jaundiced. In hospital for 4 days. Iv’s, I’ve antibiotics. That was 4 months ago. Now having the right sided pain radiating to my back. Had ultrasound which was normal. Do you think I could have SOD??
Hi Robin – sorry to hear you are not feeling well. You of course realize I am not a doctor so am not able to diagnose, treat or anything right? With that said – from what you have told me/said I would think it is entirely possible. Sounds to me like you have also had two instances of ERCP induced pancreatitis, even if your enzymes were not elevated the last time. It’s rare they don’t elevate during acute pancreatitis but it has been noted previously in case studies. I hope you feel better soon. Of course if you continue to have issues you should prod your doctor to get on the stick. 🙂
Dear Mr Healthy Guy I was diagnosed with CHRONIC PANCREATITIS and S.O.D 18 yrs ago. I was very fortunate to receive a diagnosis as after 12 surgeries, necrotic bowel and an ileostomy pouch for 6 yrs my surgeons were baffled. And I managed to get a consult with Mr Webster who was at the time the top Pacreo-Billary Professor in the World. At 1st sight it was already severe and he performed a manometry and also attempted to place stents in both my pancreatic duct and my SOD. This worked for 3-4 months until they both moved into the pancreas causing a bout of SA Pancreatitis that almost killed me. 4 months later he went in again to try to repeat the process and found the manometry incisions had made things so much worse because the body had responded by forming a huge mound of tissue around the S.O.D the size of a grapefruit so it was impossible to even see an entrance to the duct let alone find a gap big enough to fit the small tool in they use to measure the flow of digestive juices. So 18yrs later at age 46 I now find myself only able to tolerate juice supplemental drinks which are fat free and water. When I take anything else even other liquids the pain is so severe that it causes me to have symptoms similar to a mild heart attack on an ECG machine. I am also widowed with our 2 teenage daughters which makes our situation even harder. Sadly most of my medical team have given up on me. 13 yrs ago they gave me a prognosis of 1 yr max and provided us with palliative care. My GP esp seems to have given us as he has removed all the infusions I was having that kept me a measure of health saying they are only making me more comfortable and cannot cure me so are not as valuable in comparison to drugs for a cancer patient that could completely cure them. I have now fought to get my vit b12 injections back after just 6 months my b12 was dangerously low and now I’m fighting to get my vit and weekly infusions back. Previously I had weekly blood tests followed by a day each week in the hospital receiving a top up of everything my body needed specifically Magnesium, Potassium & Calcium along with a Monthly Vitamin Pouch which would instantly make me feel more alive like I could move faster.
I feel like the most important factor perhaps with any chronic condition is to remain positive and proactive willfully determined to endure and to continue to do yr best to gain accurate knowledge as to yr condition. Sadly a lot of the tests that are used for diagnostics fail because there are not enough well trained radiologists & gastro surgeons to read the results correctly. Mr Webster said my condition had advanced so quickly by all the butchers who had gone in, missed the signs in the same procedures that he did & then poked around cutting and making things worse. If I could say anything to someone without a diagnosis yet, it would be to believe in what yr body is telling u as u are the only one who feels the warning signs and do not trust any surgeon who just wants to open you up to have a look before, thoroughly checking out his history and success rates and not being afraid to ask for 2nd or 3rd opinions, as every colleague will approach things differently. Also learning as much as you can about pain control drug free alternatives. My search started with a video I thought was a hoax of a hospital in Sweden that do full open heart surgery without any anesthesia and only advanced acupuncture with pain control methods that teach you how to control pain as you would help a tantruming child.. Heat treatment has also been invaluable to my pain management. Even though they now believe i have signs of an autoimmune disease because I get constant flare ups of acute Pancreatitis with only 2 – 3 days between and my quality of life is so poor for both me and our teenage girls I can now see there are benefits I have learned from being so sick. I have learned I am so much stronger than I thought I could be, I am less selfish, more empathetic and dare I say even happier as a person than I was before getting sick because I appreciate every single blessing I receive esp the relationships I enjoy both with loved ones and with my Heavenly father.
I really want to thank you for the information you provided. It was extremely factual and you taught me things I didn’t know and is ideal to show loved ones who have formerly struggled to grasp what the illness is. It has already helped in many ways: For instance, my dietician recommended a celery juice cleanser to remove build up in my bowel from time to time which I couldn’t understand why my symptoms were heightened afterward when I consumed anything. Also I knew from experience that morphine sometimes irritates the pain further but I had not been told that it exasperated the condition further. In fact each stage my condition worsens further, the pain team continue to just raise my morphine which I have told them so many times doesn’t seem to be helping. I have talked to my consultant about the ibuprofen now and thanks to the info you provided he has done his own research and is willing to try increasing it in place of some of the morphine.
Finally I wanted to ask you about the initial prep for the food diary you suggest…because of the problems I’ve had with celery juice is there a specific treatment you recommend from yr own experience? The only time I have experienced the feeling of a clean bowel, without bloating was when I had a bariam meal. Followed by 3 weeks of nothing but water. For 7 weeks after 7 had an appetite and cut eat a variety of foods without pain. It gradually stopped working but it leaves me wondering at this late stage in the game would it be possible for me to do a regular cleanse like fortnightly or monthly so that I could eat some foods again that I can discover using the food diary that are least inflammatory to my condition. Also I would love some guidance on what food stuffs are usually least inflammatory to S.O.D if you or anyone else has ideas I can try.
My apologies for the super long text. But I cannot thank you enough for the now little Ray of hope I now feel at the end of the tunnel after enduring a particularly bad flare up with Psuedocysr which started early November and which I am still bedridden from. The loneliness u feel from enduring such a severe condition that is so unknown can be hard to endure. But with articles like these it becomes bare able again. Please accept my sincere gratitude.
Hi Shariq … I am sorry to hear you have had so much illness and pain. I don’t know what to say except if it were me I’d try to find another GP/PCP who will actually help you with the infusions that made you feel better. I don’t know who Mr. Webster is, have never heard of him but have you asked him if there was a way to remove the scar tissue without killing you? Opioids, especially morphine should not be used in patients with SOD because it causes the sphincter to spasm shut creating a backup of digestive juices that eventually enter the pancreatic duct and cause acute pancreatitis. In fact, before ERCP and newer diagnosing techniques doctors used to use the “Nardi test” which consisted of a morphine and prostigmine injection to diagnose SOD. Patients almost immediately were in pain. I see no reason why your idea of fasting would be detrimental in your case except if you are very under weight, losing more nutrients and weight could be a real problem. If you are able to buy grape seed extract and vitamin C those are very beneficial in eliminating inflammation. They may also help your pseudocyst resolve. IF possible get your doctor to ween you off the morphine which is likely doing more harm than good since you have SOD. I have a support group on facebook called beating pancreatitis support group which you may want to join. There are a number of people in there who are extensively damaged like you and quite a few have SOD as well. But that way you have have people to chat with almost 24/7. I apologize for being so late responding.